Home » Post-Operative Flexor Tendon Rehab of the Hand
Flexor Tendon Repair: Empowering Your Hand’s Road to Rehabilitation
Who is ready to flex? In this blog, we are going to detail what to expect from a post-operative flexor tendon repair of the hand.
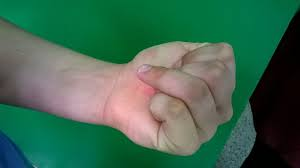
Recovering from a post-operative flexor tendon repair is often quite challenging, as the flexor tendon system in your hand is complex and constantly put under stress (Lewis, 2018). Flexor tendons of your hand run from your forearm, through your wrist and attach distally to your digits, allowing your fingers to bend inward.
What is flexor tendon ruptures?
Flexor tendon ruptures are commonly caused by lacerations or puncture wounds which can partially or completely sever these tendons. Flexor tendon ruptures caused by lacerations often have concomitant neurovascular injuries attached and therefore require immediate attention (Neiduski and Powell, 2019). Avulsion injuries can also occur when the flexor tendon is placed under high stress. Jersey finger is a good example of this, where the tendon responsible for flexing the tip of your finger is torn, resulting in an inability to bend the distal interphalangeal joint (The Hand Society, 2022).
It is vitally important to consult with a doctor or hand therapist immediately if you suspect flexor tendon damage, as they will be able to quickly identify if surgery is necessary, which in most cases, it is.
Understanding the Significance of Post-Operative Rehabilitation for Flexor Tendon Repair
Surgery will repair the tendon so it is attached throughout your hand and finger. However, your rehabilitation journey will only have just begun. Depending on the location of the injury, it may take upwards of three months for the repaired tendon to regain its previous strength and mobility (Kaskutas and Powell, 2013). Rehabilitation involves protecting your tendons from overuse to prevent further rupturing, as well as minimising scar adhesion and facilitating tendon glide and strength.
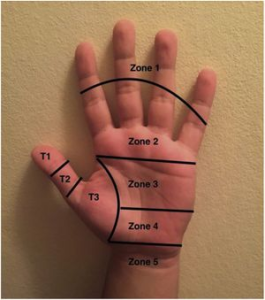
Reparation of flexor tendons in the hand can be divided into 5 zones, of which are broken down in the diagram [*Image 2].
The Importance of Post-Surgical Immobilisation for Flexor Tendon Repair
Although treatment will be specific to the zone which has been repaired, zone 1 to 5 typically follows the same principles (Physiopedia, 2022).
Post repairation, research shows that, after surgery, placing the hand in a POSI (position of safe immobilisation) splint is crucial to achieving a good outcome (Bueno et al., 2013).

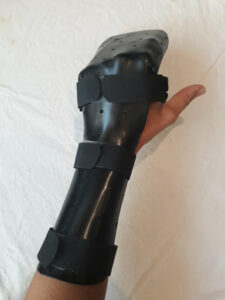
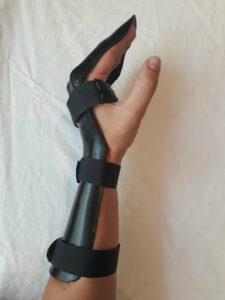
(Action rehab, 2022)
The aim of immediate post-operative treatment is to:
- Prevent tendon rupture.
- Facilitate tendon glide.
- Minimise adhesions.
- Enhance tensile strength of repair site, and
- Maximise return of hand function.
There are several protocols which are proven to be effective post flexor tendon repair. Typically, these rely on solely or a combination of passive and active range of motion. An extensive randomised control trial of 64 flexor tendon injuries found a combination of both active and passive guided mobilisation immediately post flexor tendon repair, to be more effective at restoring full function than controlled passive mobilisation (Farzad et al., 2014).
Early active and passive ranging of the repaired tendon is vital in facilitating a good outcome. A study by Tottenham et al which compared an early intervention group to a delayed intervention group showed the early intervention group had a 25% increase in the rate of desired results (Tottenham, Wilton-Bennett and Jeffrey, 1995).
So why is active and passive mobilisation important post repair?
Whenever our bodies detect tissue damage, it reacts by creating inflammation, and by laying down scar tissue (Czubryt, 2012). Scar tissue is a collective term for a group of specialised cells including fibroblasts, which begin to rapidly multiply in and around the damaged tissue in a process called cellular proliferation (Lifecare, 2022). Fibroblasts reconstruct damaged blood vessels in the area and lay down collagen to stick together and rebuild damaged tissue.
Whether your flexor tendon has been repaired or not, your body will continue to lay down scar tissue. Scar tissue is terrific at sticking your damaged site together, however a build up of scar tissue can lead to scar adhesion, which if left unchecked, can cause the collagen fibers to cross-link, shrinking tissue significantly and preventing full range of movement. By applying gentle force such as stretch, contraction, and pressure to the healing tissue, you will help reduce the occurrence of scar adhesion (Maxey and Magnusson, 2013). It is important at this stage to have frequent contact with your therapist who will work closely to determine the extent of movement relative to the risk.
Although the development of scar tissue can be a hindrance in your recovery, it is an important process experienced by everyone and needs to be respected. An exception to this lies distant but within the animal kingdom. Unlike humans, amphibians have an ability to completely regenerate their damaged tissue, meaning they regrow tissue without scar tissue formation. So, unless you’re a frog, chances are you’re likely to be stuck with a scar post flexor tendon repair (Song, Li and Stocum, 2010).
Maximize Your Flexor Tendon Repair Recovery with Consistent Hand Therapist Guidance
As you continue to improve in mobility and strength over the weeks and months, it is important that you keep in close contact with your hand therapist who will guide you throughout the length of your rehabilitation journey. A paper published in 2021 found that individuals with flexor tendon injuries who were In closer and more consistent contact with their hand therapist, were more likely to find consistency in their home exercise regime, and more likely to achieve a good outcome (Ayhan, Tuna and Oksuz, 2021).
Your rehabilitation post flexor tendon repair will be arduous. Following your therapist’s instructions are as important to your recovery as the surgery itself, so stay the course, and work with your therapist to maximise your chances of the best possible recovery.
References
Assh.org. 2022. Body Anatomy: Upper Extremity Tendons | The Hand Society. Available at: <https://www.assh.org/handcare/safety/tendons>
Ayhan, E., Tuna, Z. and Oksuz, C., 2021. Getting Better Results in Flexor Tendon Surgery and Therapy. Plastic and Reconstructive Surgery – Global Open, 9(2), p.e3432.
Bueno, E., Benjamin, M., Sisk, G., Sampson, C., Carty, M., Pribaz, J., Pomahac, B. and Talbot, S., 2013. Rehabilitation Following Hand Transplantation. HAND, 9(1), pp.9-15.
Czubryt, M., 2012. Common threads in cardiac fibrosis, infarct scar formation, and wound healing. Fibrogenesis & Tissue Repair, 5(1).
Farzad, M., Layeghi, F., Asgari, A., Ring, D., Karimlou, M. and Hosseini, S., 2014. A prospective randomized controlled trial of controlled passive mobilization vs. place and active hold exercises after zone 2 flexor tendon repair. Hand Surgery, 19(01), pp.53-59.
Lewis, D., 2018. Tendon rehabilitation: factors affecting outcomes and current concepts. Current Orthopaedic Practice, 29(2), pp.100-104.
Kaskutas, V. and Powell, R., 2013. The impact of flexor tendon rehabilitation restrictions on individuals’ independence with daily activities: Implications for hand therapists. Journal of Hand Therapy, 26(1), pp.22-29.
Lifecare. 2022. How Long Will This Take? Time Frames Of Tissue Healing | Lifecare. Available at: <https://www.lifecare.com.au/blog/how-long-will-this-take-time-frames-of-tissue-healing/>
Markiewitz, A., 2013. Complications of Hand Fractures and Their Prevention. Hand Clinics, 29(4), pp.601-620.
Maxey, L. and Magnusson, J., 2013. Rehabilitation for the Postsurgical Orthopedic Patient. Saint Louis: Elsevier Health Sciences.
Neiduski, R. and Powell, R., 2019. Flexor tendon rehabilitation in the 21st century: A systematic review. Journal of Hand Therapy, 32(2), pp.165-174.
Physiopedia. 2022. Flexor Tendon Injuries. Available at: <https://www.physio-pedia.com/Flexor_Tendon_Injuries?veaction=edit>
Savaş, S. and Aydoğan, Ç., 2022. Factors affecting orthosis adherence after acute traumatic hand tendon repairs: A prospective cohort study. Journal of Hand Therapy, 35(1), pp.32-40.
Song, F., Li, B. and Stocum, D., 2010. Amphibians as research models for regenerative medicine. Organogenesis, 6(3), pp.141-150.
Tottenham, V., Wilton-Bennett, K. and Jeffrey, J., 1995. Effects of Delayed Therapeutic Intervention following Zone II Flexor Tendon Repair. Journal of Hand Therapy, 8(1), pp.23-26.
Author
-
 View all posts
View all postsDamon Bol graduated from Deakin University with a Bachelor of Health Sciences before completing a Masters in Occupational Therapy Practice.
Damon enjoys keeping up to date with all things upper limb related, often liaising with General Practitioners, Surgeons, Physiotherapists and Occupational therapists on the latest rehabilitation techniques. He enjoys conducting independent research on contemporary and developing interventions in both surgical and conservative management of finger, wrist and elbow injuries. Furthermore, Damon conducts his on research on injury prevention and management with the aim of helping and educating his patients on how to stay safe, fit and healthy.