Home » Understanding Mallet Finger: Causes, Symptoms, and Treatment Options
Mallet finger is a common injury that can cause significant pain and discomfort. It occurs when the outermost joint of the finger is injured, usually from a forceful impact or accident. The condition can cause the fingertip to droop and prevent it from straightening, making even simple tasks difficult. In this blog, we will discuss the causes, symptoms, and treatment options for mallet finger. By understanding this condition, you can take the necessary steps to manage it and regain hand function.
What is Mallet Finger?
When discussing finger injuries, one of the most common to occur is the mallet finger. When dissecting the mechanism that causes this injury, the most common mechanism of injury in mallet finger is a sudden flexion of the DIP joint with the resistance force directed along the long axis of the finger. This leads to terminal extensor tendon tear or tendon avulsion with a bony fragment.
Mallet finger leads to an imbalance in the distribution of the extensor force between the proximal interphalangeal (PIP) and DIP joints. If left untreated, mallet finger leads to a swan neck deformity from PIP joint hyperextension and DIP joint flexion.
Soft-tissue vs Bony
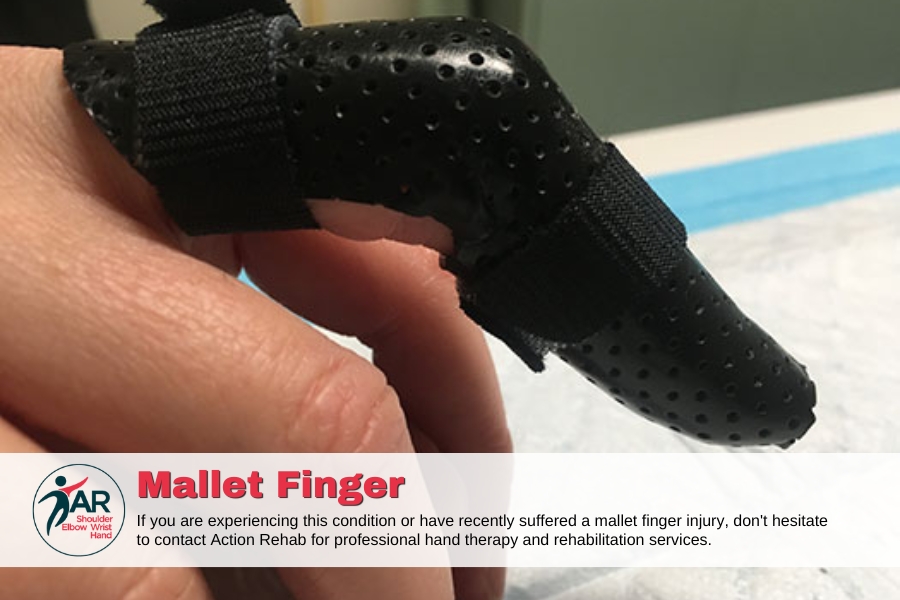
Early signs of a mallet finger include:
- Swelling
- Bruising
- Redness
- An inability to straighten your fingertip
- Tenderness
- A detached fingernail
- Redness under the fingernail bed
Soft-tissue mallet’s can be quite complex and requires consistent patient compliance to ensure a positive result is meet as little as 1 mm of terminal tendon lengthening resulted in −25° of DIP joint extension lag. This means adjusting exact tension during orthosis making is crucial (Schweitzer & Rayan, 2004). Once the extension force by the central slip and lateral bands overcomes the flexion force by the superficial and deep flexor tendon across the proximal interphalangeal joint, a Swan neck deformity is created (Laramus & Matthew, 2017)
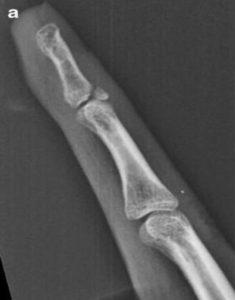
In contrast, *Figure A shows a bony avulsion following a football injury which led to a DIP lag of 26 degrees and was told only surgery could fix the issue. However, following being placed in an anti-swan orthosis for six weeks, his lag reduced to zero. Many bony avulsions are considered ‘stable’ with surgery rarely being a suitable option.
Mallet Finger Treatment Options
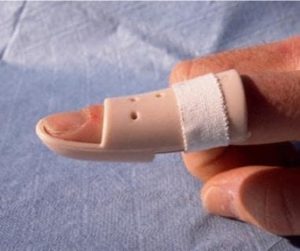
Examination of imaging is the initial step in determining the severity and future conservative management. When the symptoms of a mallet finger are present, an x-ray will be sufficient to determine the type of injury. Once the type of mallet is known, this introduces the immobilisation process which will involve positioning enough tension across the extensor tendon to allow the healing process to begin.
Multiple splints are available to treat mallet fingers however, many of which can lead to permanent deformity if not positioned correctly. The most effective form of splinting comes from a thermoplastic approach positioning the finger in an anti-swan position which will include approximately 50-70 degrees of the PIP joint and slight hyperflexion at the DIP (Mclinot, 2008). Once immobilised, the patient will need to wear the splint full-time for 8-12 weeks before beginning active movements into flexion.
In addition, the patient will be introduced to a specific task to ensure the lag reduces and the skin care of the finger is maintained. As mentioned previously, the complex nature of this injury relies on the compliance of the patient to determine whether a great result is achieved (Anderson, 2011).
Final thoughts on mallet finger and its treatment options
In conclusion, mallet finger can be a painful and frustrating injury, but it is treatable with the right care and attention. We hope this article has provided you with a better understanding of mallet finger injuries, their causes, symptoms, and available treatment options.
If you’re experiencing any of the symptoms mentioned above or have recently suffered a mallet finger injury, don’t hesitate to contact Action Rehab for professional hand therapy and rehabilitation services. Our experienced hand therapists will create a personalised treatment plan tailored to your needs to help you regain hand functionality and strength. We also offer second opinion consultations for those who are unsure about their current treatment plan or seeking alternative options. Contact us today to book an appointment and take the first step towards your hand recovery.
References:
- Stark, H. H., Boyes, J. H., & Wilson, J. N. (1962). Mallet finger. JBJS, 44(6), 1061-1068.
- Schweitzer, T. P., & Rayan, G. M. (2004). The terminal tendon of the digital extensor mechanism: Part II, kinematic study. The Journal of hand surgery, 29(5), 903-908.
- Mclinot, C. L. E. B. (2008). A mallet injury case study with recommendations for practice. The British Journal of Hand Therapy, 13(1), 21-26
- Lamaris, G. A., & Matthew, M. K. (2017). The Diagnosis and Management of Mallet Finger Injuries. HAND, 12(3), 223–228. https://doi.org/10.1177/1558944716642763
Author
-
 View all posts
View all postsBen Cunningham is the Hand Therapist at the Melbourne Football Club and has over 20 years’ experience providing hand and upper limb therapy, including working in the United Kingdom at the Queen Victoria Hospital and as the senior clinician at The Alfred Hospital in Melbourne.